The bandage is attached to the ankle distractor with a surgical clamp and adjusted as needed to provide the desired amount of joint distraction ( Fig 2).

Our preference is to achieve joint distraction with a moistened 2-inch-wide cotton conforming bandage (Covidien, Mansfield, MA) fashioned with a tension loop around the hallux at the level of the first web space. The limb is exsanguinated before the sterile Guhl noninvasive distractor (Smith & Nephew, Andover, MA) is attached. Dorsomedial and dorsolateral portals are marked at the level of the MTP-1 joint approximately 0.5 cm from the edges of the extensor hallucis longus to avoid injury to the dorsomedial cutaneous nerve and terminal branches of the deep peroneal nerve ( Fig 1). The extensor hallucis longus tendon and MTP-1 joints are palpated and marked on the skin. The extremity is prepared and draped to the level of the tourniquet. A well-padded calf tourniquet is used to optimize visualization during the procedure. A bump using rolled blankets is often positioned under the ipsilateral hemi-pelvis to orient the axis of the foot perpendicular to the floor. The procedure is performed with the patient in the supine position using a split-leg extension with the heels at the edge of the bed to maximize access to the operative extremity. Step 1: Preoperative Planning and Patient Positioning We present our technique for arthroscopic assessment of the MTP-1 joint in general, as well as treatment of OCLs of the proximal phalanx specifically ( Video 1). Thus MTP-1 joint arthroscopy may facilitate improved intra-articular access and visualization. Regarding the MTP-1 joint specifically, the curved surfaces of the metatarsal head and proximal phalanx base limit visualization of and access to the entire joint with open approaches. 1, 2, 3 Even though studies comparing arthroscopy-based techniques with open techniques for management of MTP-1 joint pathology are lacking, arthroscopy-based procedures in general have the benefit of less bleeding, decreased infection risk, improved cosmesis, and abbreviated recovery periods. Although the indications for MTP-1 joint arthroscopy continue to evolve, its use for management of mild to moderate hallux rigidus, osteochondral lesions (OCLs), loose bodies, arthrofibrosis, synovitis, and sesamoid conditions, as well as drainage of septic joints and gouty tophi, is most common. Use of these techniques for addressing various conditions of the first metatarsophalangeal (MTP-1) joint has gained in popularity over recent years.

Ultrasound and MR will show both.Advances in small-joint arthroscopy have enabled surgeons to treat intra-articular pathology through a minimally invasive approach while mitigating iatrogenic injury. Diagnostic injections are the simplest method of differentiating the two pathologies (Miller 2001).
#Mtp joints series
Indeed, Coughlin's series of neuromas had about 5% of patients who also had instability, and about the same proportion of Peck's MTP instability patients also had neuromas. It may be difficult to distinguish the pain of MTP instability from that of an interdigital neuroma. The Thompson draw test demonstrates instability with the MTP joint flexed slightly and the proximal phalanx drawn up and down. Instability, subluxation or dislocation of the MTP joint – probably about 10-20% present with fixed dislocation.Hammertoe and/or crossover toe deformity.Tenderness around the joint, especially under the plantar plate.Puffiness around one or more MTP joints (usually the second), sometimes with divergence of the toes.toe deformity with predominantly pressure symptoms, but where MTP instability influenced treatment.pain related to the index MTP joint which may then decrease and be partly replaced by a feeling of walking on a pebble and toe deformity.generalised forefoot pain - like many patients with metatarsalgia, there are often multiple factors such as reduced ankle dorsiflexion, first ray insufficiency and toe deformities.Peck et al identified three main patterns of symptoms: There is a strong association with hallux valgus.
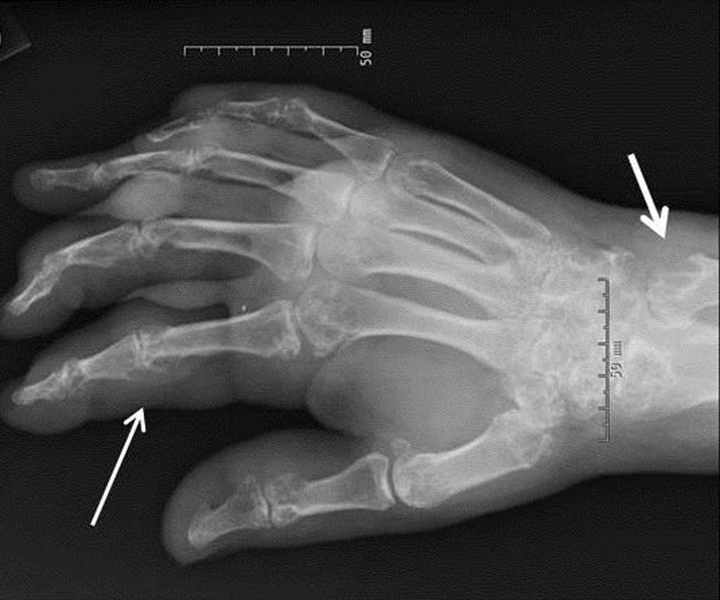
Most patients have no history of trauma or inflammatory arthritis. The typical patient is a middle-aged woman.
